Back to School and Right Back Home Again: Kids at Risk for More Than COVID-19
Children Are at Higher Risk of Respiratory Illness This Year
The high rate of COVID-19 circulation in the U.S. as we head into winter leads to concerns, again, about a possible “twindemic” of flu and COVID-19. Unlike last year though, if the “twindemic” arrives, it may hit children the hardest. Adults have been eligible for vaccination for months, and many are still working from home and limiting social interactions. But millions of kids have returned to school for in-person learning, and children under 12 years old are not yet eligible for COVID-19 vaccination. And already, dozens of schools have had to shut down due to outbreaks of COVID-19. The majority of states do not have mask mandates for schools, and several states have banned mask mandates, leaving schools with higher risks and fewer options to keep kids safe.
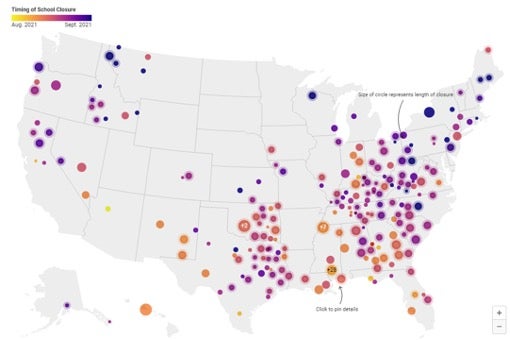
Outbreaks of COVID-19 in schools will continue until the pandemic can be brought under control through greater population immunity. The Delta variant is currently responsible for more than 99% of infections of SARS-CoV-2,1 the virus that causes COVID-19. The American Academy of Pediatrics publishes a weekly report tracking SARS-CoV-2 infections in children. Currently, the level of community transmission of SARS-CoV-2 in the U.S. is high,1 with 300 cases per day per 100,000 residents. In the first week of September alone, almost 250,000 infections were reported in children.2
The bottom line: Unlike last year, children increasingly are getting sick from COVID-19. Right now, children represent our most vulnerable segment of the population because of limited vaccine coverage and greater social interactions as a result of being back in school. In addition, unique challenges brought on by the pandemic, such as missed vaccinations and fewer pathogen exposures due to social distancing measures, may put them at higher risk for other respiratory illnesses as well.
Children are more likely than adults to be infected with multiple respiratory viruses at once
Prior to the pandemic, researchers at the Cleveland Clinic conducted a study to see how frequently people are infected with more than one respiratory virus at the same time. Among a sample of over 1,000 respiratory infections, almost 1 in 5 children were infected with more than one virus at the same time.3 Children were infected with multiple viruses 6 times more frequently than adults were. The reason for this is simple: young children do not have the immune experience that adults do; their immune systems have not encountered as many viruses as adults have. This increases the chances that kids will get infected with multiple viruses at the same time.
This summer, we observed off-season outbreaks of a common and sometimes serious respiratory disease, respiratory syncytial virus (RSV). The high levels of community transmission of SARS-CoV-2, the coming cold and flu season, in addition to other respiratory pathogens like pertussis (the bacterium that causes whooping cough), will increase the likelihood of co-infections in children this year. Even last year, with schools and businesses closed and influenza circulation brought to historically low levels, as many as 3.2% of, or 1 in 30, children infected with SARS-CoV-2 were infected with influenza at the same time.4
We are entering another uncertain flu season
“Reduced population immunity due to lack of flu virus activity since March 2020 could result in an early and possibly severe flu season” — Centers for Disease Control and Prevention (CDC).
In the U.S. currently, influenza cases are higher this year than at the same time last year. As we have started our reopening process, respiratory viruses like RSV have returned as well. Delayed vaccinations during the pandemic, combined with children going back to school, have placed children in an unusually risky position. While it is true that children are generally more protected from severe outcomes from COVID-19, influenza and other co-illnesses may put them at greater risk of hospitalization and death.
We must use every tool we have to protect children this year
Since flu viruses can live and spread to people from surfaces for up to 48 hours, and SARS-CoV-2 can live on surfaces from hours to days,5 CDC recommends routing cleaning and disinfecting of frequently touched surfaces such as desks, toys, door knobs, and faucets and counters in restrooms.6 We recommend using disinfecting wipes on high-touch and frequently used surfaces throughout the day, and more thorough disinfecting at night using electrostatics.
This year, it’s not just about COVID-19. The conditions of the pandemic have put children at an increased risk of illness from bacterial and viral pathogens. Vaccination, hand hygiene, wearing masks, staying home when ill, and routine cleaning and disinfection are all going to be needed together to keep kids in school, healthy, and safe.
Download the K–12 Environmental Cleaning and Disinfection Protocol Guide
For the latest information on COVID-19 and variants, visit our CloroxPro COVID-19 Hub.
REFERENCES
1. CDC Covid Data tracker. Centers for Disease Control and Prevention. Retrieved September 20, 2021, from https://covid.cdc.gov/covid-data-tracker/#variant-proportions.
2. Children and covid-19: State-level data report. American Academy of Pediatrics. Retrieved September 20, 2021, from https://www.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/children-and-covid-19-state-level-data-report/.
3. Mandelia, Y., Procop, G. W., Richter, S. S., et al. (2021). Dynamics and predisposition of respiratory viral co-infections in children and adults. Clinical Microbiology and Infection, 27(4).
4. Dao, T. L., Hoang, V. T., Colson, P., et al. (2021). Co-infection of SARS-COV-2 and influenza viruses: A systematic review and meta-analysis. Journal of Clinical Virology Plus, 1(3), 100036.
5. Wißmann, J. E., Kirchhoff, L., Brüggemann, Y., et al. (2021). Persistence of pathogens on inanimate surfaces: A narrative review. Microorganisms, 9(2), 343.
6. How to clean and disinfect schools to help slow the spread of flu. Centers for Disease Control and Prevention. Retrieved September 20, 2021, from


