The COVID-19 pandemic has brought unprecedented changes to healthcare throughout the world. Fraught with high volumes of patients and paucity of resources and testing, combined with personal protective equipment (PPE) and staffing shortages the past year has taught the healthcare community lasting lessons in resilience. The rapidly advancing knowledge around the SARS-CoV-2, the virus that causes COVID-19, has also prompted a shift in the standard of care. In the face of such multifaceted challenges, the world of Infection Prevention and the capacity to monitor and prevent healthcare-associated infections (HAIs), changed.
How, why, and what changes have occurred?
Stevens et al described the impact on HAI prevention efforts as notable due to diversion of human resources for surveillance and case identification, process measures for prevention of HAIs (such as hand hygiene), mitigation resources (lack of real-time feedback), and the lack of adequate supplies of PPE for traditional HAIs resulting in potential increased risk of cross-contamination.
The transmission of SARS-CoV-2 lacked clarity, but was described to spread via aerosol and surface contamination in 2020. Infection prevention resources were critical in this environment of uncertainty, both for adequate disinfection of surfaces, but also for appropriate use of PPE. Although the overall risk of surface contamination resulting in transmission of SARS-CoV-2 was ultimately deemed to be low, effective disinfection practices were still necessary, adding to the workload burden of already overstretched infection prevention teams.
Furthermore, the level of illness of patients affected by COVID-19 combined with the limited PPE resources, resulted in changes in patient care that could be unpredictable at times. In clinical care settings for example, the long length of hospital stay, particularly in the intensive care unit (ICU), was accompanied by longer durations of support devices, such as endotracheal tubes, central venous catheters (CVCs), and urinary catheters. The longer duration of which increased the numbers of opportunities for in the failure of executing process measures to prevent HAIs.
The increased use of prone positioning, even amongst non-ventilated patients, may have negatively impacted visible access to many dressings and device sites for several hours per day. Finally, with PPE limitations, many adjustments were made to decrease required trips and time spent in patient rooms, such as transitioning intravenous medication pumps to outside of patient rooms. Such changes may have positively impacted PPE utilization rates, but may have carried negative counterbalances with increased risks of HAIs due to lack of direct visualization, longer tubing with possible increased risks of contamination, and potential preference for more durable catheters, such as CVCs to minimize risk of dislodgement or need for new access placement. Finally, it was would be remiss to not acknowledge that all of the above were further augmented by the fear and anxiety that resulted from the many unknowns and struggles faced by healthcare workers, and may have increased the risk for error.
What was the result?
The data is still evolving, but increased rates of HAIs have been reported. Amongst the critically ill, one study showed a 46% increase in HAIs, with ventilator-associated pneumonia (VAP) and central line associated bloodstream infections (CLABSIs) as leading causes. Interestingly, within this group, only the intubated patients were noted to have HAIs. A review similarly showed several studies with increased CLABSIs amongst patients with COVID-19, as compared to those without. Moreover, a study of CLABSI data from the National Health Safety Network as similarly demonstrated a 28% increase in CLABSI from early in the pandemic. Of interest, Clostridiodes difficile rates have decreased in some studies, without concurrent decreases in antibiotic use, highlighting that strong infection prevention measures including environmental cleaning and use of PPE and handwashing remain critical in the prevention of nosocomial spread of this infection.
So, where do we go from here?
We must recognize the impact the pandemic has had on healthcare, with rapid changes in practice, high work burdens with increasing burnout, and the need to move forward. Hardwiring our HAI prevention practices to ensure consistency in both the best and worst of times is critical. Considering how to identify, implement and amplify the positive innovations and changes throughout the field is necessary. Of paramount importance is ensuring robust infection prevention teams have adequate resources for surveillance, mitigation, education and quality improvement.
Thank you to all of the tireless Infection Prevention teams, continuing to strive to provide the safest care for our patients and healthcare teams around the world!
This is the fourth post of a six-part blog series, Infections Inside Out, by Dr. Kelly Cawcutt. Read part three here.
The rise of antibiotic resistance is one of the greatest threats in healthcare today. According to the Centers for Disease Control and Prevention (CDC), every year in the United States approximately 2.8 million people develop an infection from antibiotic-resistant bacteria and over 35,000 people die.
"She was in her 70s when she was admitted to the hospital with sepsis. Her right hip was infected, and unfortunately, this was not the first infection. Two years prior, she had fractured her femur and developed osteomyelitis. She had several prior hospitalizations, but they were all in another country. Now, cultures were obtained from the head of the femur and yielded Klebsiella pneumoniae. This member of the Enterobacteriaceae family is usually easily killed by many antibiotics. However, this time testing showed that not only did this bacteria demonstrate resistance to a powerful class of antibiotics known as carbapenems (due to the presence of New Delhi metallo-betalactamase (NDM), but even more frightening, it was resistant to all other antibiotics available. The patient ultimately succumbed to septic shock."
- Chen, Lei, et al. "Notes from the Field: Pan-Resistant New Delhi Metallo-Beta-Lactamase-Producing Klebsiella pneumoniae-Washoe County, Nevada, 2016." MMWR. Morbidity and mortality weekly report 66.1 (2017): 33-33
How did this happen?
In truth, this has always been happening. Since the discovery of penicillin in 1928, we have been faced with the reality of the ongoing evolution of antibiotic resistance. So much so, that in his Nobel lecture, Sir Alexander Fleming addressed the risk of resistance if caution was not used in the administration of penicillin.
"But I would like to sound one note of warning. Penicillin is to all intents and purposes non-poisonous so there is no need to worry about giving a penicillin overdose and poisoning the patient. There may be a danger, though, in underdosage. It is not difficult to make microbes resistant to penicillin in the laboratory by exposing them to concentrations not sufficient to kill them, and the same thing has occasionally happened in the body. The time may come when penicillin can be bought by anyone in the shops. Then there is the danger that the ignorant man may easily underdose himself and by exposing his microbes to non-lethal quantities of the drug make them resistant."
- Sir Alexander Fleming, Nobel Lecture, 1945
Since the onset of our first antibiotic, we have continued to see bacteria with resistance to antibiotics, including within 1–2 years from the release of the antibiotic to the description of the new resistance. Based on this, the CDC publishes a report on the biggest antibiotic-resistant threats in the U.S. The 2019 report has 18 pathogens listed as either an urgent, serious or concerning threat. Several of these bacteria will be familiar to you from prior posts — Methicillin-resistant Staphylococcus aureus (MRSA) and Carbapenem-Resistant Enterobacteriaceae (CRE), C. diff, and Candida auris (C. auris). Others, such as carbapenem-resistant Acinetobacter and multi-drug resistant Pseudomonas aeruginosa are of urgent and serious concern, respectively, and still play significant roles in many healthcare-associated infections (HAIs).
What can we do about it?
With multiple antibiotic resistant organisms (AROs) threatening human health, focusing on prevention of continued resistance is of paramount importance. This profound public health threat resulted in a national action plan for combating antibiotic-resistant bacteria in 2015. Key aspects of this plan include improving antibiotic stewardship and adherence to infection prevention and control strategies.
Sir Alexander Fleming had it right — inappropriate use of penicillin, or any antibiotic, can result in resistance. And just as resistance has been with us since the discovery of penicillin, so has unnecessary antibiotic use. Approximately 30% of antibiotics given in US hospitals are inappropriate - based on suboptimal choice or unnecessary overall. Yet, we know that it is exposure to antibiotics that drives the evolution of resistance, and not just exposure of antibiotics to a single individual. Overuse of antibiotics in a hospital, or ward, may portend resistance to multiple patients.
Therefore, improving antibiotic use through stewardship principles is a critical step towards preventing further antibiotic resistance. The CDC has published Core Elements of Hospital Antibiotic Stewardship Programs, yet uptake of these principles is incomplete. The Infectious Diseases Society of America (IDSA) has also published guidance for implementing stewardship programs. Additionally, the Centers for Medicare and Medicaid Services have instituted requirements for antimicrobial stewardship, further highlighting the importance of this intervention. Finally, each healthcare professional can join in public health advocacy for stewardship through the CDC U.S. Antibiotic Awareness Week (scheduled for November 18-24, 2021).
But, combating antibiotic-resistant with stewardship is not enough. Infection prevention and control practices synergistically help prevent ongoing spread of these organisms. Practices that decrease the bioburden of bacteria from the environment, including from the hands of healthcare workers, are absolutely necessary. These strategies then decrease the likelihood of transmission of AROs from one patient to another. From hand hygiene to transmission-based precautions to decrease transmission of multidrug resistant organisms (MDROs) to environmental cleaning and disinfection, infection prevention and control is quintessential in the fight against antibiotic resistance.
Thankfully, Antibiotic Resistant Doesn’t Mean Disinfectant Resistant
Monitoring for these organisms within the facility aids in recognition of possible developing outbreaks and assists in determining where the transmission may have occurred. For instance, the Agency for Healthcare Research and Quality (AHRQ) has a toolkit to assist with CRE control and prevention, which would have been a critical component for preventing both the infection and death of our patient above.
As part of these programs, we must recognize that environmental contamination with AROs or MDROs, is an essential weapon in this fight. Ensuring that the physical environment is clean, specifically frequently touched areas, cannot be understated in importance.
As infection prevention and control professionals, it is imperative that we recognize the profound threat that antibiotic resistance plays in our fight against HAIs. With inevitable use of antibiotics during our lives, we are all at risk and we all need to do our part to wage war on these formidable foes.
Kelly Cawcutt, MD, MS, FACP is a paid consultant for Clorox Healthcare.
This is the third post of a six-part blog series, Infections Inside Out, by Dr. Kelly Cawcutt. Read part two here.
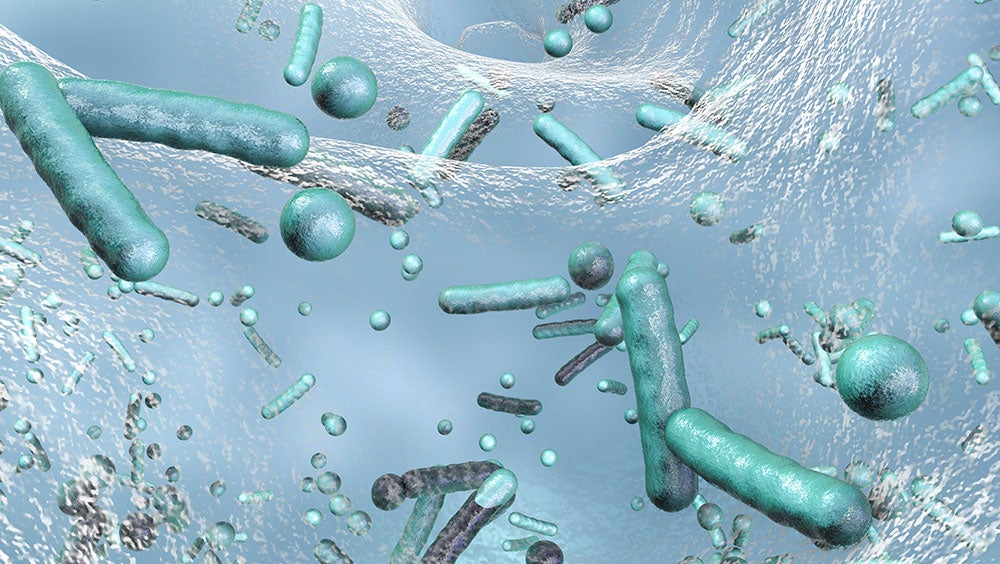
Biofilms play an important role in the development of hospital-acquired infections (HAIs). In my line of work, I’m often reminded of their presence when handlining central venous catheters or endotracheal tubes, but biofilms can also be present on any environmental surfaces. Biofilms are defined as a complex collection of microorganisms that attach to a surface and create a surface specific ecosystemic on that surface (known as an extracellular polymeric substance [EPS]). Given the complexity, and strong adherence to surfaces, biofilms result in a perpetual conglomerate of microorganisms that may be impossible to fully eradicate, resulting in a difficult, albeit often underestimated cause of infections in healthcare.
Given the increase usage of ventilators for the treatment of severe COVID patients, I thought now was a particularly good time to drive awareness about this complex, Jello-like matrix filled with microorganisms such as bacteria.
Biofilms contribute to many infectious diseases. Some classic examples are endocarditis, prosthetic joint infections and Clostridiodes difficile (C. diff) along with device-related infections such as central line-associated bloodstream infections (CLABSIs), catheter-associated urinary tract infections (CAUTIs) and ventilator-associated pneumonia (VAP), among others. In the era of COVID-19, the impact of biofilms on HAIs may be more prominent due to the high device utilization in the intensive care units (ICUs) and long length of stays.
Considering the impact of biofilms, there are many details to keep in mind. First, given the capacity for biofilms to form on any surface, preventing microorganisms from attaching to a surface is a key intervention. The prevention of infection is multifaceted, and echoes the importance of infection control measures such as hand hygiene, device stewardship, aseptic technique, maintenance of devices and equipment, and environmental cleaning. Beyond this, patients may have additional risk factors that contribute to their likelihood of biofilm development which can include diabetes, kidney disease and immunosuppression. The risk factors are associated with decreased innate immune responses that normally fight the development of biofilms, so when a disease impacting the innate immune system is present, there is less of our individual capacity to prevent the build-up of that "gunk" on my patient’s endotracheal tube. Recognizing the role comorbid conditions, especially those that are very common (like diabetes and kidney disease) may play in such infections is essential as we strive to beat biofilms and prevent HAIs.
There are many human pathogens that are described to comprise, and grow within, biofilms can result in infection, including, but not limited to, Staphylococcus aureus, Pseudomonas aeruginosa and Legionella pneumophila. Candida species, including both Candida albicans and Candida auris (C. auris), are known to also cause biofilms. The known presence of these organisms has resulted in innovative devices, such as central venous catheters, impregnated with antimicrobial agents to prevent microbial attachment to the catheter, and therefore biofilm development. Such catheters have demonstrated decreases in HAIs, specifically in this scenario, CLABSI.
Although individual patient infection control measures must be followed, environmental sources of biofilm cannot be ignored. One specific rising concern in the infection control world is C. auris, which was first detected in 2009, and subsequently has spread throughout the world. Infections secondary to C. auris are significant due the life-threatening nature of these infections, combined with both the resistance to several antifungal medications and the capacity to spread within healthcare facilities. C. auris has been described to cause surface biofilms in patient rooms that may be difficult to eradicate, therefore be a conduit for infections. C. auris may be contracted from a patient, or their environment (including equipment that may be used for multiple patients), in as little as 4 hours, therefore effective disinfection is critical. Chlorhexidine-based regimens for patient asepsis may not be as effective as povidone iodine and environmental disinfectants, such as ethyl alcohol and quaternary ammonium, may be less effective than hydrogen peroxide or sodium hypochlorite. We must understand which infection control strategies, including the chemicals used, are effective against pathogens, or we will miss the opportunity to prevent HAIs!
Beyond the patient and physical environment, biofilms with infectious pathogens (such as Pseudomonas aeruginosa and Legionella pneumophilia) can form in water sources and clear guidance exists from the CDC on how to assess, and decrease the risk, of water-based biofilm as a source for transmission of infection within hospitals. Examples of where such biofilms could occur is within faucets, ice machines, showers, toilets and drains.
Given the near impossibility of eradicating biofilms, further research into prevention of biofilms is of paramount importance. Specifically, the roles of antimicrobial impregnated devices and surfaces (such as the central venous catheter device mentioned above), and optimal patient asepsis and environmental disinfection. Our best offense continues to be adherence to infection control practices and engaging the entire healthcare team in the one-two punch required to beat biofilms. Our patients are depending on us!
Kelly Cawcutt, MD, MS, FACP is a paid consultant for Clorox Healthcare.
This is the second post of a six-part blog series, Infections Inside Out, by Dr. Kelly Cawcutt. Read part one here.
Hospital-acquired infections (HAIs) are infections acquired during medical care and are often directly related to the use of medical devices or procedures, along with lapses in critical infection control practices such hand hygiene, and appropriate cleaning and disinfection. Every day in the U.S., approximately 1 in 31 patients will suffer from a HAI. These infections can include central line associated bloodstream infections (CLABSI), catheter-associated urinary tract infections (CAUTI), surgical site infections (SSIs), ventilator-associated pneumonia (VAP) and development of Clostridiodes difficile infection (CDI). The Centers for Disease Control and Prevention (CDC), along with State and county health departments, along with individual hospitals, monitor these closely via reports to the National Healthcare Safety Network, which assesses outbreaks and monitors progress towards future prevention efforts — with a goal of elimination of HAIs in the future of medicine.
The impact of COVID-19 on HAIs may ultimately be profound due to the use of antibiotics for possible bacterial co-infection and prolonged ICU stays, including the use of multiple invasive devices placing these vulnerable patients at risk for CLABSI, CAUTI, VAP, CDI. Additional factors clearly impacting HAIs during this pandemic include lack of appropriate resources and supply chain issues (such as personal protective equipment and testing supplies), combined with varying rates of infected healthcare workers and risk of burnout impacting the available workforce. Finally, there is ongoing concern that fear amidst this pandemic may negatively impact adherence to infection control practices. Never has prevention of HAIs been more critical given the burden of COVID-19 on healthcare around the world.
Prevention of HAIs
Prevention of HAIs is comprised of several key concepts: avoid both device placement and antibiotic use unless clearly indicated, remove devices and stop antibiotics as soon as possible, and follow infection control measures for the healthcare workers and environment (such as standard and transmission-based precautions, hand hygiene and environmental and equipment cleaning).
With the clear impact of HAIs, there are several different guidelines focusing on how to prevent HAIs. A few critical recommendations and guidelines are:
- The Society for Healthcare Epidemiology of America’s compendium of strategies to prevent HAIs
- CDC guidelines for preventing HAIs
- WHO guidelines for infection prevention
Anyone within the healthcare field, including the patient, is accountable to help prevent HAIs. This is truly a multidisciplinary effort!
Patient’s Role
In the end, we are all patients and, as mentioned above, can play a role in prevention of HAIs. There are several key actions anyone can take to keep ourselves, and our loved ones, safe from these infections. Practicing excellent hand hygiene, watching closely for signs of developing infection, remembering to only take antibiotics when your healthcare team feels it is necessary and remaining an advocate for safety throughout your hospital stay (such as reminding healthcare workers to perform hand hygiene). (Here is a quick video on five tips to prevent HAIs as a patient.)
Device-Related Risks
There are many invasive devices that are frequently used for patient care, and once they are in place for at least 48 hours, those devices carry the risk for a possible reportable HAI to develop. Some patients require infusions of medications or frequent access to blood draws and monitoring, therefore may have a central venous catheter placed, thereby creating a simultaneous risk for developing CLABSI. Certain patients will have trouble urinating, or need very close monitoring of urine output due to impaired kidney, so an indwelling urinary catheter is inserted and, with that, the risk for CAUTI arises. Patients with severe lung disease, such as those with respiratory failure from COVID-19, may require invasive mechanical ventilation, as provided via an endotracheal tube. Much like the two catheters listed above, with insertion and use of the endotracheal tube, the risk for development of VAP evolves.
In essence, all of these devices are inserted through a potential non-sterile source and therefore carry a risk for bacteria to create a biofilm on the external surface of the catheter, or have bacterial inoculated on the internal surface during cares, increasing the risk of a possible life-threatening HAI. Understanding appropriate indications, insertion techniques, maintenance and prompt removal, once no longer indicated, is of paramount importance.
Environmental Cleaning
Infections can spread within the healthcare setting, including based on inadequate environmental cleaning. CDI is one such infection, which is highlighted below. Additionally, there are many aspects of the environment to consider, such as the high touch surfaces at risk for contamination based on lack of hand hygiene. Air-based contamination are based on infectious aerosols (which may additionally occur via coughing, sneezing, flushing a toilet, procedures for a patient that may generate aerosols such as suctional or intubation) or mold secondary to construction or other damage. Water-based contamination can be found in ice machines, faucets, drains and with equipment that utilizes water but is not maintained or cleaned via manufacturer instructions-for-use (IFUs).
All of these simple components around us can serve as conduits for infection. Although this may be top of mind for many during this pandemic and tempt us to focus only on COVID-19, the more ‘mundane’ aspects of environment infection control are just as important in 2020 as they were each year prior. It’s critical that healthcare team members, including nurses, doctors, technicians and EVS staff responsible for cleaning equipment, or the environment, use products that are EPA-registered to be effective against these HAIs.
Seeing C. diff Differently – What Has Changed in Prevention?
CDI is the most common cause of HAIs in the U.S., with specific guidelines for infection prevention given its prevalence from national societies (Infectious Diseases Society of America and the Society of Healthcare Epidemiology of America) and from the CDC. There are several key steps to preventing CDI as a HAI:
- Antibiotic use is the primary driver for development of CDI, therefore it is imperative to follow antibiotic stewardship principles to minimize risk of development of CDI.
- Implement contact precautions for those with confirmed or suspected infections, to avoid unintended spread to others.
- Consider use of innovative engineering for improving adherence to isolation precautions with solutions such as the "Red Box."
- Maintain appropriate personal protective equipment with gowns, gloves and hand washing (especially in outbreak settings) to prevent spread of spores.
- Confirm with appropriate testing strategies. This is key as colonization exists with this organism, so non-infectious etiologies should be considered, do not test if laxatives have been used in the last 48 hours, do not send solid stool for testing and remember that repeat testing for cure is not necessary.
- If non-disposable equipment is used, dedicating equipment to the patient room should be done if possible. If there is an inadequate equipment supply, cleaning before and after each patient use should be done. For CDI, even if using a 2-in-1 product, cleaning should occur prior to disinfecting and should be completed with a compatible sporicidal disinfectant (EPA List K agents; such as Clorox Healthcare® Bleach Germicidal Wipes) should be utilized.
- Terminal room cleaning for patient rooms in which C. diff was present is also critical to prevent ongoing spread of infection as the spores can survive for months within the hospital room and many standard disinfectants are ineffective, therefore effective disinfection is critically important, especially during outbreak situations. Methods may include cleaners, such as Clorox Healthcare® Bleach Germicidal Disinfectants or Clorox Healthcare® Fuzion® Cleaner Disinfectant.
Despite all the efforts on COVID-19, as frontline healthcare teams, we must all pitch in to continue the fight against HAIs. Our patients are depending on us.
Kelly Cawcutt, MD, MS, FACP is a paid consultant for Clorox Healthcare.
This is the first post of a six-part blog series, Infections Inside Out.
Infectious diseases remain a critical cause of morbidity, mortality and cost in all healthcare facilities including outpatient clinics, long-term care facilities and acute care facilities, such as hospitals. Infections can come from two main places – inside the hospital walls and from outside within a community. A patient can develop a community-acquired infection prior to arrival in any healthcare setting, which often is what prompted the patient to seek care. The most recent example of this is COVID-19 (SARS-CoV-2). This virus is impacting healthcare facilities around the world with increased patient burdens and human-to-human spread in which infected patients are transmitting the infection to other patients, visitors and healthcare workers.
There are also many healthcare-associated infections (HAIs) that patients in both acute and long-term care settings are at specific risk for based on multiple factors such as: having chronic medical problems that increase possible risks (such as requiring dialysis or conditions causing weakened immune systems), prior admission to healthcare facilities or receipt of antibiotics (placing patients at increased risk of acquisition of antibiotic-resistant (AR) infections or Clostridiodes difficle (C.diff) infection, the use of invasive devices (such as a ventilator in the setting of respiratory failure), and any procedures (such as surgery) needed for medical care. Lapses in infection control practices such as hand hygiene and cleaning and disinfection are another HAI risk factor. Going forward, we will specifically focus on HAIs in acute healthcare settings.
The primary reported infections under the umbrella of HAIs include central line associated bloodstream infections (CLABSI), catheter associated urinary tract infections (CAUTI), and surgical site infections (SSIs) and ventilator associated pneumonia (VAP), and C. diff gastroenteritis (actually the leading cause of HAI). These HAIs are reported and tracked nationally by the National Healthcare Safety Network (NHSN). However, it is important to note that these infections can be caused by both antibiotic-susceptible and AR pathogens. According to the CDC, each year in the U.S., there are over 2.8 million infectious causes by AR pathogens. This results in over 35,000 deaths. Microorganisms that are frequently also discussed in this category include C. diff infections and detection of AR bacteria, such as Carbapenem-resistant Enterobacteriaceae (CRE) or Methicillin-resistant Staphylococcus aureus (MRSA). Prevention of these infections is clearly of paramount importance and infection control practices such as adherence to guidance for hand hygiene, isolation practices, when to wear gloves and gowns and environmental cleaning, to prevent spread throughout the hospital. Additional infection control expert guidance is available through many organizations including the CDC, Society for Healthcare Epidemiology of America (SHEA) and the Association for Professionals in Infection Control and Epidemiology (APIC).
The toll that infections can have on patients, and healthcare facilities as a whole, can be daunting when you consider the needs for ongoing surveillance, diagnosis, management and complex infection prevention strategies. Strategies for the prevention of HAIs nearly all start with maintaining excellent hand hygiene, minimizing unnecessary invasive devices, prudent and correct use of antibiotics, employing appropriate precautions to prevent spread of infection within a facility and correct and thorough environmental and equipment cleaning and disinfecting to help eliminate pathogens. In many ways, the strategies are easier said than done; however, they are important to helping prevent the spread of the pathogens that cause infection, especially when you consider the substantial cost, they have on patient health and hospital cost.
Over the next posts, we will break down some of the key aspects of infectious diseases and prevention in the acute healthcare setting, including AR, HAIs, biofilms, multi-drug resistant organisms and challenges of infection prevention. Together, we can all strive to better understand and improve infection prevention thereby improving patient safety and care.
Kelly Cawcutt, MD, MS, FACP is a paid consultant for Clorox Healthcare.