
If you work in healthcare, it's likely that you’re pretty familiar with healthcare-associated infections (HAIs), such as Central Line-associated Bloodstream Infection (CLABSI), Surgical Site Infection (SSI), Catheter-associated Urinary Tract Infections (CAUTI), and Ventilator-associated Pneumonia (VAP). These are all infections associated with medical devices that are often necessary but can lead to life-threatening complications.
Preventing HAIs
Prior to the COVID-19 pandemic, the CDC reported that mandatory healthcare reporting of HAI’s showed improvements in the rates of various HAIs. However, during the first 2 years of the COVID-19 pandemic, many hospitals reported increases in HAIs. This was likely a result of several rounds of enormous ‘surges’ in patient volume, sicker patients who required longer stays and periods of intubation, central lines and urinary catheters, staffing and supply shortages as well as alterations in infection prevention practices.
As we move into the next stage of the pandemic, with less invasive management options and shorter hospitalizations, many clinicians are looking to circle back to the basics of infection prevention. As the CDC and CloroxPro resources show, infection prevention is a ‘team sport’ that involves engagement from everyone in a healthcare facility. From surface decontamination by Environmental Services (as well as by non-EVS staff) in the form of decontaminating used equipment and high-touch surfaces in workspaces, to monitoring adherence to disinfection protocols by Infection Prevention, to liaising with clinical staff to determine the necessity of “tubes and drains,” all staff have a vital role to play in keeping patients safe.
A Team Effort
The team dynamic that was so critical during the early days of the COVID-19 pandemic (the “all-hands-on-deck”/“everyone has a crucial role” mentality), once again is a huge part of keeping HAIs at bay. As a hospitalist, I love this aspect of working in health care settings, (whether I’m at the hospital, or skilled nursing facility, or clinic), where the people you work with can set the tone for the day and will routinely save you from yourself! This is why I try to do team rounding on Intensive Care Unit (ICU) patients, so that, hopefully, a team member will ask “is the central line still necessary?” while another clinician might say “can we possibly discontinue the urinary catheter?” to help guide patients safely through their hospital course without picking up any HAIs along the way.
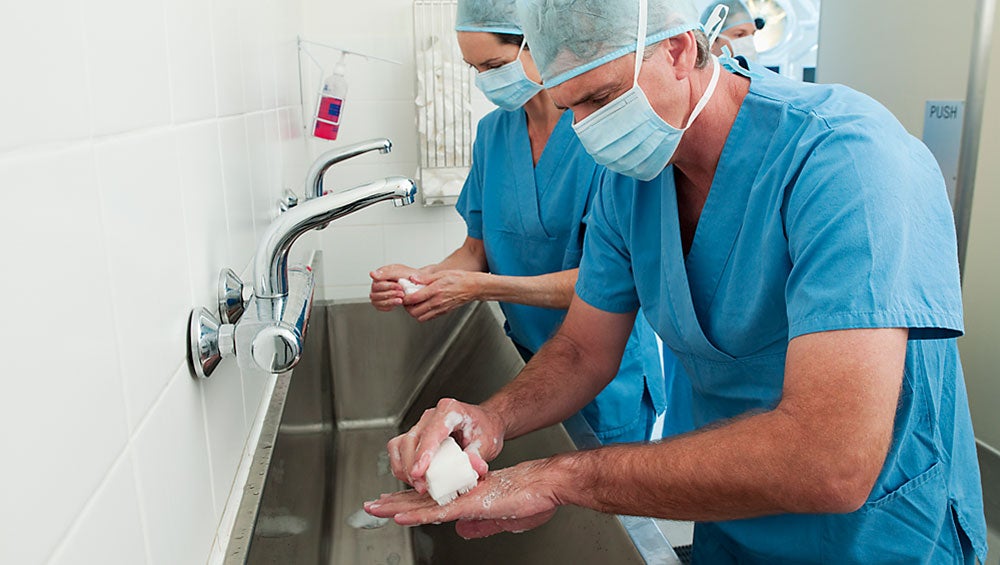
For HAIs where surface contamination is a major source of spread (such as C. diff), thorough handwashing as well as attention to surfaces is key. In terms of decontamination of surfaces and devices, CloroxPro has many resources to help steer healthcare facilities as they try to say “see you later” to HAIs.
Unlike the pandemic, HAIs are not “unprecedented,” and we know exactly what we need to do to minimize their presence in the healthcare environment. After navigating the uncertainty and fear of the early pandemic, I personally feel a bit of relief when I think about returning (with my healthcare teammates) to the basics of HAI prevention.
Originally published by FierceHealthcare.
As a physician working at a busy hospital in New York City, my days were already frantic pre-pandemic.
Prior to March 2020, I knew we had an infection prevention (IP) team, but I had no understanding of the scope of their responsibilities. Once my hospital became part of the epicenter of the COVID-19 outbreak, it was all hands on deck and I gained a greater sense of the role IP plays.
I wish I had had an earlier introduction to IP’s activities, as it surely would have been beneficial in my practice as a hospitalist. To overcome COVID-19 in NYC, the physician staff and IPs came together to tackle many obstacles.
A key learning point from the pandemic is that we need to integrate our teams more within the hospital walls to work collaboratively as one team. Below are six tips to maximize the critical relationship between clinicians and IPs for pandemic events and for the general working day.
- Know the difference between the infectious disease (ID) consult service and the infection prevention (IP) team. This might sound simple, but at the peak of COVID-19 in New York City both played a key role in the management of the pandemic. These two groups were getting nonstop calls, pages and emails. But while ID’s role is to consult on a complicated COVID-19 case, IP was responsible for managing isolation protocols, tracing contacts and advising on infection prevention best practices.
- Get to know the IP team. If you are a clinician working in the hospital setting, chances are that IP is just down the hall from your workroom. Matching a face to a name is always helpful, but it was even more essential during the COVID-19 ramp-up when NYC clinicians were in constant contact with the IP team. One bonus of meeting the IP team is that they might even give you their cellphone number, which was a luxury item during the pandemic.
- Check in daily. During pandemic times workflows can become chaotic. Think: constant faxes from the Department of Health and frequent pings from hospital leadership. Make a plan to touch base with IP at least once a day to confirm that you are on the same page. This way you can"‘round" on current isolation needs, hear the most updated recommendations on personal protective equipment (PPE), etc.
- You don’t know what you don’t know. Your hospital’s IP team members are the local experts on isolation and infection control. During COVID-19, standards for isolation and PPE evolved quickly, so we needed to ensure my clinical team and I had the most accurate and current data. Our IP team scheduled just-in-time trainings to keep us all safe and up-to-speed. Don’t be shy about seeking out these learning opportunities.
- See one, do one, teach one. This is an old medical axiom, but for these purposes I would suggest that you try to make introductions early and often. Medical trainees and new clinical staff may not be familiar with IP, so if you see an IP team member on the floors or in the cafeteria, by all means, make the introduction. A resident may have received many pages from that IP specialist, but connecting with them in real life can "level up" the relationship. Too often we remain "silo-ed" in our own specialties. This can be a way to teach new staff excellent interprofessional teamwork.
- Never let a crisis go to waste. There are so many lessons to be learned from different stages of the pandemic response. If something isn’t working in your relationship with IP, ask “is there something I can do differently?” During the early days of the COVID-19 response in New York we frequently had to reassess our workflow to determine the best ways to engage with IP. These disruptions can be really productive when they uncover new approaches or systems.
While the COVID-19 crisis in the spring in New York was not something I would ever wish for, I hope we can learn from the experience and bring more interprofessional collaboration into our work in the future.
Integrating the clinical and IP teams is just one way to get this started.
Grace Farris, MD is a paid consultant for Clorox Healthcare.